This post is part of our In Case You Missed It series, revisiting research and analysis from Serif’s 2025 State of the Data report. The underlying shift it describes—toward transparency-enabled repricing at scale—has only accelerated.
A Question That Wasn’t Answerable—At Scale
For most of the history of employer-sponsored healthcare, answering a basic question—are we paying the right amount?—has been operationally impractical.
Claims are complex. Rate structures are embedded in proprietary contracts. And reconstructing what should have been allowed for any individual claim has historically required manual effort—making full-book validation infeasible.
So organizations worked within those constraints. Payment integrity firms audited subsets of claims based on rules or thresholds. TPAs and employers relied on contracted rates without a clear way to validate them independently. Benefits consultants modeled alternatives using benchmarks rather than claim-level data.
The limitation wasn’t analytical sophistication. It was access to usable rate data.
Price transparency changes that.
What “Repricing at Scale” Actually Means
Price transparency data makes it possible to take a full set of claims and recalculate expected allowed amounts using publicly posted negotiated rates—at the CPT, DRG, and facility level—across specific providers and networks.
In practice, this enables two distinct but related capabilities:
- Claim validation: Comparing what was paid or billed on a claim to what posted negotiated rates would support
- Scenario modeling: Repricing those same claims under alternative networks or carrier configurations
Why This Matters Now: A Full-Book Audit Layer
The most immediate traction for transparency-enabled repricing has been in payment integrity—because it solves a fundamental limitation in how claims are audited.
Traditional audit models are sampling-based. Claims are flagged based on thresholds, outliers, or known patterns, and only a subset is reviewed. Everything else goes unexamined.
Repricing at scale introduces a different model:
- Every claim for a given provider or system can be evaluated
- Allowed amounts can be benchmarked directly against posted rates
- Variances can be identified systematically—not just when flagged
This enables a new class of audit questions:
- Where do paid amounts exceed what negotiated rates would support?
- Where are billed charges inconsistent with contractually expected structures?
- Which providers or facilities show persistent variance across the full claim population?
- Are discrepancies isolated—or systemic?
Instead of identifying issues opportunistically, organizations can track variance across the full book of business.
From Audit to Insight: Expanding the Surface Area
Once repricing is applied consistently across all claims for a system, the same dataset begins to support broader analysis.
What starts as validation becomes visibility.
- Payment Integrity
Full-book repricing allows firms to move beyond sampling-based audits toward continuous, population-level validation—without the cost structure that historically made that infeasible.
This supports:
- Systematic variance detection
- Provider-level audit tracking
- Identification of repeat patterns across CPTs, DRGs, and facilities
- Network Strategy
Using the same claims, organizations can model:
- Total allowed spend under different networks
- Facility-level variation within a system
- Service lines driving 20–50% cost deltas
This allows decisions around carrier selection and network design to be grounded in actual utilization rather than generic benchmarks.
One of the reasons this analysis is particularly powerful is that it combines two different types of data: historical claims and current negotiated rates. Claims show what has already happened—but they are inherently backward-looking. Price transparency data reflects current contracted rates, which means repricing enables organizations to project costs forward using up-to-date pricing rather than relying solely on historical spend. That distinction matters in environments where rates are changing and where decisions—like network selection or renewal—depend on understanding not just past costs, but what those costs will look like going forward.
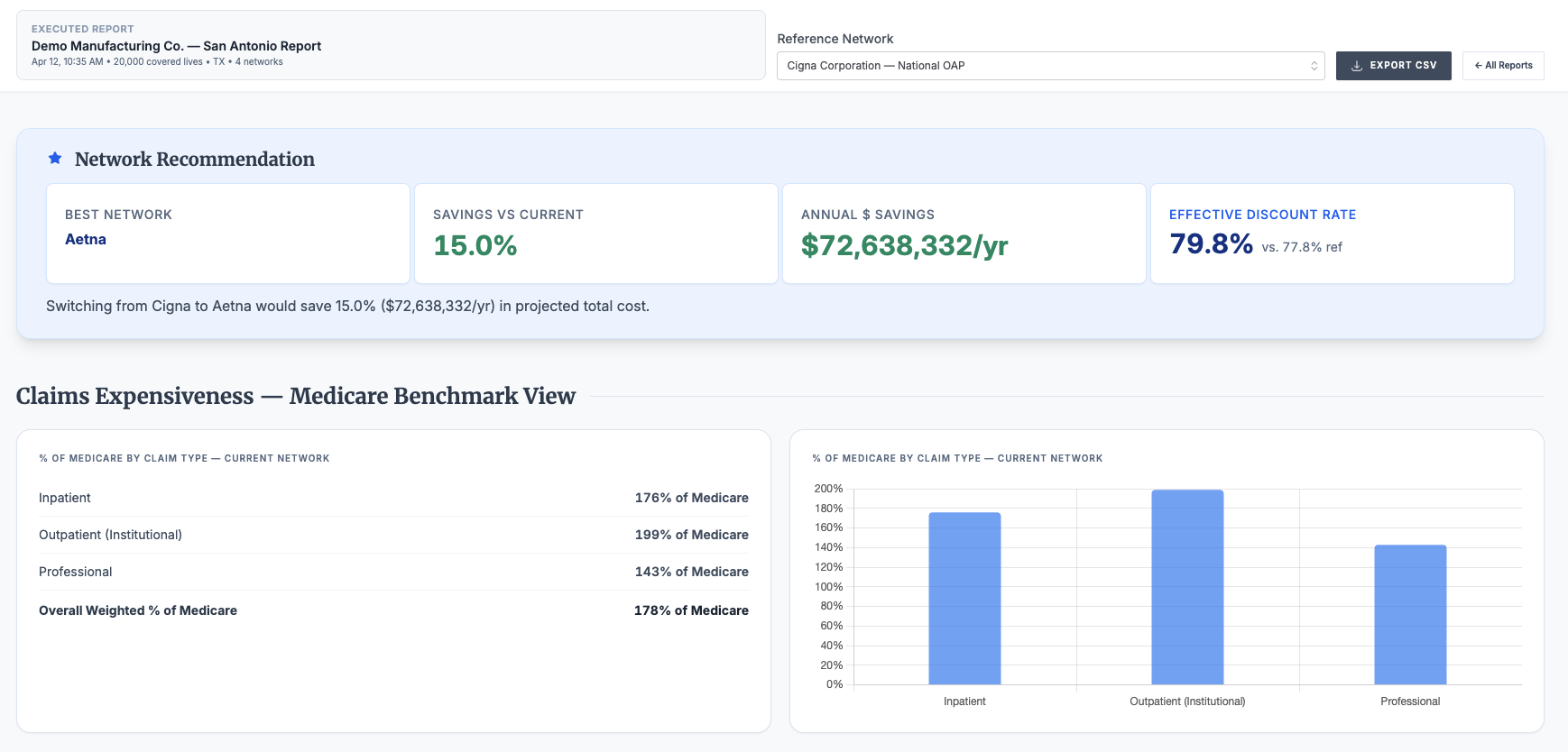
This quantifies how network choices shape spend for the specific facilities where members actually receive care—and surfaces variation across campuses or affiliated facilities within the same system that would otherwise be invisible.
- Advisor & Consultant Support
Benefits consultants can move from directional estimates to claim-grounded modeling, giving them:
- A defensible way to quantify network tradeoffs
- Stronger data to support client recommendations
- Differentiation in competitive advisory environments
A Structural Shift in What Repricing Does
Traditionally, repricing was:
- Retrospective
- Selective
- Manual
At scale, it becomes:
- Continuous (applied across all claims)
- Comparative (anchored to posted rates across networks)
- Actionable (usable for both audit and decision-making)
The same underlying capability now supports:
- Claim validation
- Variance tracking
- Network modeling
- Strategy development
That’s a different category of functionality—not just a more efficient audit tool.
How Serif Supports This Work
The value of repricing depends on the quality and usability of the underlying data.
Serif aggregates and normalizes payer transparency files at scale—resolving inconsistencies across payer schemas, deduplicating implausible records, and aligning negotiated rates to the CPTs, DRGs, and revenue codes present in claims.
This allows:
- Direct claim-to-rate comparison for validation workflows
- Accurate recalculation of allowed amounts across network scenarios
- Consistent analysis across providers, facilities, and service lines
Because this process is automated, teams can move from raw data to usable outputs in days—not weeks of manual reconstruction.
The result is a scalable, defensible view of how claims align—or diverge—from expected rates, and how those patterns translate into broader cost dynamics.
Where This Is Going
Transparency-enabled repricing is still early—but the direction is clear.
What began as a way to validate individual claims is becoming a foundational layer for both audit and strategy.
As more organizations adopt it, full-book repricing will become a standard input into:
- Payment integrity workflows
- Network and carrier evaluation
- Benefit design decisions
Not because the questions are new—but because, for the first time, they can be answered comprehensively.
Want to Learn More?
For organizations exploring how to apply transparency-enabled repricing to their own data, Serif can run targeted analyses across key providers or systems—demonstrating both claim-level variance and system-level impact in a matter of days. See it in Signal or drop us a line at hello@serifhealth.com.

